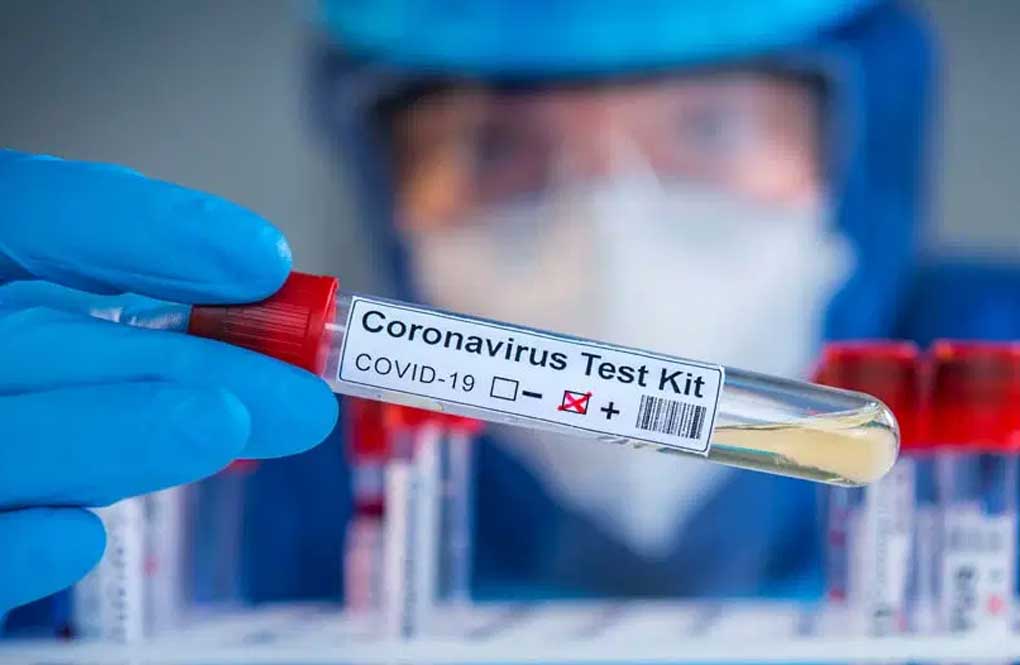
WASHINGTON — A widely used coronavirus test is under scrutiny this week after federal health officials warned that it could deliver inaccurate results if laboratory technicians don’t follow the the latest updates from the manufacturer.
The Food and Drug Administration’s warning over Thermo Fisher’s TaqPath test underscores the complexity of COVID-19 tests and how easily they can be skewed by faulty processing and equipment.
The FDA action follows a report last month by Connecticut public health officials that the test resulted in at least 90 people receiving false positive results for the coronavirus.
WHAT HAPPENED WITH THE TEST?
Thermo Fisher’s test is one of the standard tools used to screen for COVID-19, run on large, automated machines found in many U.S. hospitals and laboratories. The FDA flagged two separate issues that could potentially result in false results: the chemical mixing process and computer software that runs on the company’s machine. Thermo Fisher has provided new instructions for mixing. And a software update fixes the second problem, the FDA said.
For all positive results, FDA said labs should review the instrument settings.
Thermo Fisher said in a statement that its data shows the issues are rare and most users get accurate results by following company directions.
HOW ACCURATE ARE COVID-19 TESTS?
No test is 100% accurate and all medical tests are expected to deliver a certain small portion of false results. Less is known about the accuracy of COVID-19 tests because of how quickly they were rushed through the regulatory process because of the pandemic.
Thermo Fisher’s test uses molecular technology that is considered the gold standard for detecting the COVID-19 virus and other viruses. The test uses chemicals to extract the genetic material of the virus from a nasal swab, then amplifies it many times until it is detectable with a computer.
Thermo Fisher’s test was among the first granted emergency use by the FDA in mid-March. Like other companies, it got the OK based on laboratory experiments it submitted to regulators. The test successfully detected coronavirus in 60 lab-made samples of the virus, and successfully ruled out the virus in 60 samples that didn’t contain the virus. That was sufficient to meet FDA requirements..
However, experts have warned that these laboratory measures are very different from the large patient studies that assess the real-world performance of a test. Those studies can reveal factors that can skew results, such as faulty samples or incorrect processing .
HOW SIGNIFICANT ARE FALSE RESULTS?
The biggest concern during infectious disease outbreaks is usually avoiding false negatives, or when the test fails to catch people who are actually infected. That can result in some people unknowingly spreading the virus.
But Dr. Albert Ko of Yale’s School of Public Health noted that false positives can also create problems, particularly in places like nursing homes and prisons where people are grouped together based on test results.
“You may wind up putting someone who hasn’t been infected together with people who may be infected and are contagious,” Ko said.
Test results can be affected by a variety of factors, including the type of test used, the quality of the sample and when it was taken during the course of any infection.
(AP)