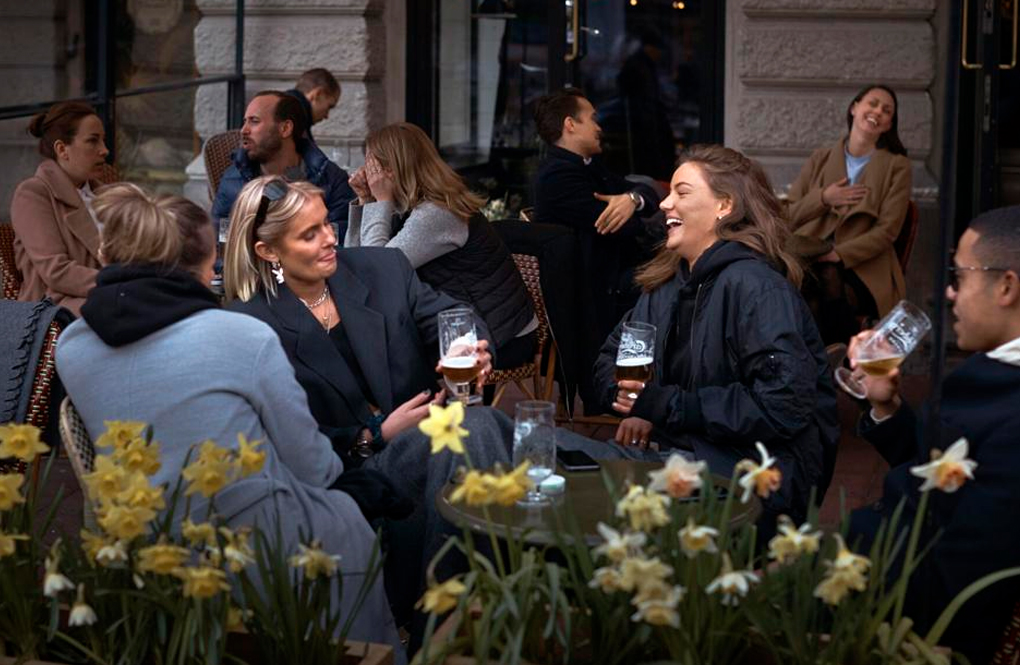One in five Australians say pressure to pay the bills at the height of the pandemic, when the nature of jobs drastically changed, adversely affected their mental health, a new survey has found.
Researchers from University of Sydney and Australia’s Mental Health Think Tank have surveyed more than 1000 Australians in the last two years.
The participants ranged in age from 18 to 89 and answered questions about their mental health experiences during the height of the pandemic when lockdowns were the norm.
The responses, published in the journal PLOS ONE last month, found the pandemic had “pressurised” existing triggers for poor mental health by amplifying financial stress and reducing social support and connection.
Around 20 per cent of participants said financial hardships, with rampant lay-offs and the inability to work from home in frontline jobs, forced many to work while sick with the virus and affected their mental health.
Almost 10 per cent of participants said the pandemic fragmented their social networks, which in turn led to them feeling more socially isolated and disconnected.
Melbourne was one of the most locked-down cities globally, with people there enduring more than 260 days confined to their homes.
Many in the survey, conducted between July to December 2020 and March and June 2021, said the prolonged break in connecting socially with people had a long-term impact on getting out again and mixing with the outside world.
Lead author Marlee Bower said the mental health experiences of the general public were largely unknown.
With prolonged lockdowns, many sought mental health support for the first-time in their lives but faced multiple barriers to access.
“Many respondents said accessing the current mental health support system was expensive and difficult to navigate,” she said.
It was “compounded by the community and political stigma about what it means to be unemployed, receive welfare or mental health support”.
She noted how an “already overloaded mental health sector” was stretched with “fewer available spots for new patients and long waitlists”.
The researchers argued a more holistic approach across various government departments was needed for mental health policymaking.
(AAP)