Young Victorian children who become primary close contacts will be allowed to return to childcare after seven days, as long as they perform a rapid COVID-19 tests for 14 days.
It comes as Victoria’s chief health officer has criticised the national cabinet’s COVID-19 roadmap for failing to mention what will happen in the pandemic “recovery phase” and called for more federal funding.
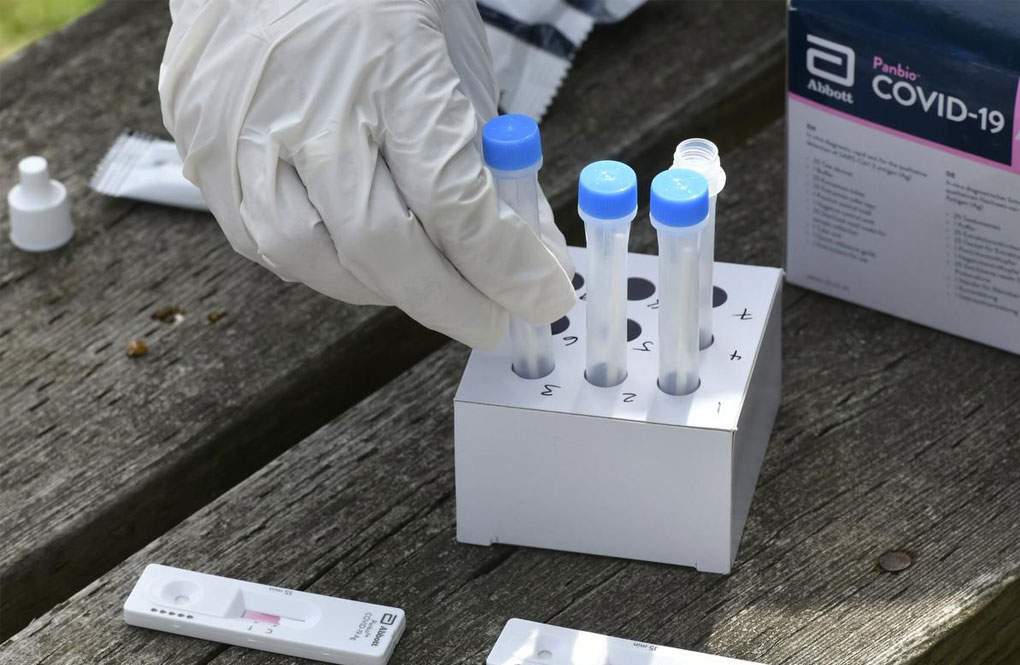
The Victorian government will distribute free rapid antigen testing kits to kindergartens and long daycare centres this week to help manage COVID-19 outbreaks in early childhood services.
From Monday, eligible kindergartens and long daycare services are invited to opt into a program to receive at-home rapid antigen tests for kids identified as primary close contacts.
This will halve quarantine for those children to seven days, with kids allowed to return to early childhood services after quarantine if they test negative to COVID-19 in a PCR test on day six.
To attend childcare again, children must return negative rapid antigen tests each they attend a service, from days eight to 14.
Families must report the test results to their childcare provider each morning before attending.
Children under 12 are not yet eligible for a COVID-19 vaccine and under current rules must quarantine for 14 days if they are a close contact.
Victoria’s case numbers dropped to 905 local COVID-19 infections on Sunday, about 300 fewer than the previous day, and four people died.
Chief Health Officer Brett Sutton and health economist Stephen Duckett have penned an editorial in the Medical Journal of Australia on the need for a “recovery phase” in the national pandemic plan.
A recovery phase would address economic effects and manage mental health impact of the pandemic, they say.
“Disappointingly, the (national cabinet) roadmap includes no explicit recovery phase; it as if we could all soon heave a sigh of relief and simply move on,” the article says.
“The recovery phase needs to rebuild community and system resilience and redress disadvantage exacerbated by COVID-19.”
Recovery would allow planning for workforce responses, prepare for worker burnout and staff recovery.
It would also include lessons from the pandemic across government, hospitals and primary care services, to discover “what went well, what went badly”.
“From a public health perspective, this should not be a witch hunt, but rather an exercise in learning and improvement,” the article says.
They called for the federal government to share in the health costs caused by the pandemic, “not just the direct costs … but also the costs of deferred care in 2022 and possibly even 2023”.
Decision makers should spend early 2022 “assessing and developing strategies” to respond to problems brought on by the pandemic, including health system delays, mental health impact, long COVID and health worker burnout, they said in the article.
Monday signals a vaccine deadline for residential aged care workers, who must be fully vaccinated against COVID-19 to continue working.
(AAP)