One of the great mysteries of the coronavirus is how quickly it rocketed around the world.
It first flared in central China and, within three months, was on every continent but Antarctica, shutting down daily life for millions. Behind the rapid spread was something that initially caught scientists off guard, baffled health authorities and undermined early containment efforts — the virus could be spread by seemingly healthy people.
As workers return to offices, children prepare to return to schools and those desperate for normalcy again visit malls and restaurants, the emerging science points to a menacing reality: If people who appear healthy can transmit the illness, it may be impossible to contain.
“It can be a killer and then 40 percent of people don’t even know they have it,” said Dr. Eric Topol, head of Scripps Research Translational Institute.
Researchers have exposed the frightening likelihood of silent spread of the virus by asymptomatic and presymptomatic carriers. But how major a role seemingly healthy people play in swelling the ranks of those infected remains unanswered — and at the top of the scientific agenda.
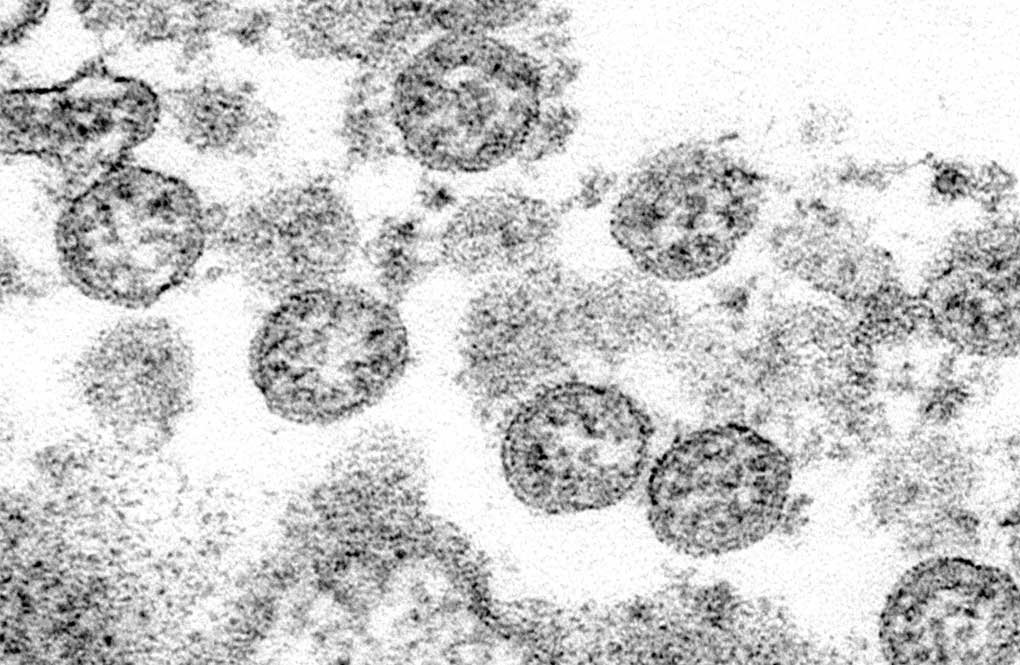
The small but mighty coronavirus can unlock a human cell, set up shop and mass produce tens of thousands of copies of itself in a single day. Virus levels skyrocket before the first cough, if one ever arrives. And astonishing to scientists, an estimated 4 in 10 infected people don’t ever have symptoms.
The slyness of the virus remains on the minds of many scientists as they watch societies reopen, wondering what happens if silent spreaders aren’t detected until it’s too late.
Travelers with no coughs can slip past airport screens. Workers without fevers won’t be caught by temperature checks. People who don’t feel tired and achy will attend business meetings.
And outbreaks could begin anew.
THE FIRST HINTS
As early as January, there were signs people could harbor the virus without showing symptoms. Still, many scientists remained unconvinced.
The concept of people unwittingly spreading disease has never been an easy one to grasp, from the polio epidemic of mid-century America to the spread of HIV decades later.
As COVID-19 emerged, health officials believed it would be like other coronaviruses and that people were most infectious when showing symptoms like cough and fever, with transmission rare otherwise.
“We were thinking this thing is going to look like SARS: a long incubation period and no transmission during the incubation period,” said Lauren Ancel Meyers, a disease modeler at the University of Texas at Austin.
Behind the scenes, scientists like Meyers were sharing their alarming finding with health officials. By scouring the websites of Chinese health departments, Meyers and her team found more than 50 cases between Jan. 21 and Feb. 8 where the person who brought the virus home didn’t develop symptoms until after infecting a family member.
“When we looked at the data, we said, ‘Oh no, this can’t be true,’” Meyers said. “It was shocking.”
CLUES ON A CRUISE SHIP
Rebecca Frasure, who contracted the virus while aboard the Diamond Princess cruise, sat in bed in Japan in late February, frustrated to be kept hospitalized even though she didn’t have any symptoms.
“I’m perfectly healthy except having this virus in my body,” Frasure said.
Without widespread and frequent testing, it’s impossible to know how many people without symptoms might carry it. The Diamond Princess, which idled in the Port of Yokohama while the virus exploded onboard, enticed researchers.
A mathematical model built by the London School of Hygiene and Tropical Medicine aimed at estimating how many infected people without symptoms were being missed indicated that a startling three-quarters of infected people on the Princess were asymptomatic.
In Washington state, similar clues emerged for Dr. Jeff Duchin as a team of investigators examined the Life Care nursing home — the site of the first major U.S. cluster of cases — and found health care workers were spreading the virus to other elder care facilities. They believed at least some were working while infected but before feeling symptoms.
In March, more than half the residents at another nursing home who tested positive didn’t have symptoms.
All that underscored the need to shift gears and acknowledge the virus couldn’t be totally stopped.
“This disease is going to be extremely hard to control,” Duchin recalled thinking.
UNANSWERED QUESTIONS
The nose and mouth are convenient entryways for the coronavirus. Once inside, the virus commandeers the cell’s machinery to copy itself, while fending off the body’s immune defenses. Virus levels skyrocket in the upper airway, all without symptoms early on. Many scientists believe that, during these days, people can spread virus just by talking, breathing or touching surfaces.
In the truly asymptomatic, the immune system wins the battle before they ever feel sick.
As it became clearer that healthy people could spread the virus, U.S. health authorities opted not to wait for scientific certainty. In early April, the Centers for Disease Control and Prevention recommended people wear masks.
Days later, Chinese researchers published a paper saying patients are most infectious two to three days before developing symptoms. Evidence continues to accumulate, and the CDC now estimates 40% of transmission is occurring before people feel sick.
Still, doubt remains among scientists, most notably among the World Health Organization, which has discounted the importance of asymptomatic infection, though it recently began to acknowledge that possibility and advised people to wear masks.
U.S. health officials blame China for delays in sharing information on silent spread. But Topol contends the U.S. could have mounted its own testing program with viral genome sequencing.
That’s no small matter: Gaining scientific clarity earlier would have saved lives.
“We’ve been slow on everything in the United States,” Topol said. “And I have to say it’s shameful.”
Associated Press writers Maria Cheng in London and Victoria Milko in Jakarta, Indonesia, contributed to this story.